Etiology: Clostridium perfringens and Clostridium difficile are Gram-positive, spore-forming anaerobic bacilli. These anaerobic bacteria produce toxins that cause edema and hemorrhage, and occasionally mucosal dysfunction and necrosis.
Incidence: The incidence of clostridial enteritis is moderate.
Transmission: C. perfringens and C. difficile are transmitted by the fecal-oral route, and overgrowth is precipitated by factors that disrupt gut flora.
Clinical Disease: Diarrheal disease in hamsters with cecal bacterial dysbiosis results from dietary changes, antibiotic therapy, concurrent diseases or other physiologic stressors that can disrupt the cecal microbiota. Antibiotics implicated in clostridial enteritis include lincomycin, erythromycin, penicillin, ampicillin, gentamycin, vancomycin and cephalosporins.
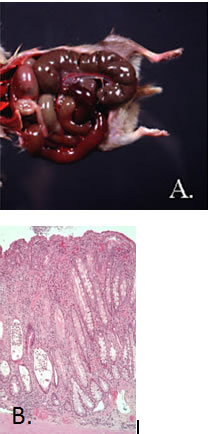
Pathology: In acute disease, lesions are typical of enterotoxemia. Gross lesions include serosal and mucosal hemorrhages of the cecum and sometimes the lower intestine (A.). Enterocyte degeneration with sloughing, mucosal edema, hemorrhages and variable neutrophilic infiltrate may be observed microscopically (B.).
In chronic disease, gross lesions include mild dehydration and thickening of the cecal wall with thick to watery cecal contents. The cecal mucosa is hyperplastic with variable lymphoplasmacytic inflammatory cell infiltrate.
Diagnosis: Definitive diagnosis can be made by identification of the bacteria in anaerobic cultures of ileal or cecal contents or by detection of the iota-like toxins (toxin A and B of C. difficile) in cecal filtrates. PCR can also be used for diagnosis.