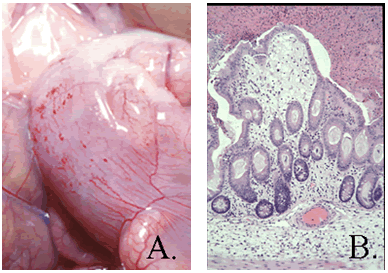
Pathology: Gross lesions include fluid cecal contents with serosal hemorrhages and edema on the cecum, and occasionally the ileum and proximal colon (A). Microscopically, there is necrotic erosive or ulcerative typhlitis with swollen or vacuolated enterocytes, pseudomembrane formation, heterophilic infiltration, as well as submucosal edema and hemorrhage (B). Large Gram-positive bacilli are present on the mucosal surface.
Diagnosis: Diagnosis of Clostridial species can be made by performing a Gram stain on impression smears and collecting feces for toxin analysis, culture, and PCR. Gross and microscopic lesions are characteristic but not diagnostic.